What is known?
Despite Australia’s National Cervical Screening Program, Indigenous women have a disproportionately high burden of cervical cancer.
Compared to non-Indigenous women, higher numbers of screened Indigenous women also have high-grade cervical abnormalities (HGA), that can indicate a true precancerous cervical lesion that could potentially develop into invasive cervical cancers.
What is new?
Results based on more than 2 million women (around 47,000 Indigenous) who had a Pap test showed a significantly higher number (prevalence) of screened Indigenous women had a histologically confirmed HGA (hHGA) than non-Indigenous women. This differential remained after adjustment for age group, area-level SES, remoteness, and Indigenous population (%), although the magnitude reduced over time.
Prevalence was lower in older women and higher for women from outer regional and remote/very remote areas.
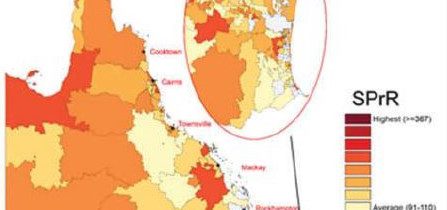
Spatial analysis also suggested that hHGA prevalence was consistently higher among Indigenous women in small geographical areas across Queensland.
What does this mean?
The decrease in Indigenous-non-Indigenous differential in hHGA prevalence is encouraging. Further research into the key drivers of the continuing higher numbers among Indigenous women is needed.
Given that human papillomavirus infection (HPV) is necessary for developing cervical abnormalities, the lack of contemporary data on HPV infection by Indigenous status following the introduction of national HPV vaccination program in 2007 as well as information on HPV vaccination rates highlight key data limitations.
Contact: Paramita Dasgupta
Reference: Dasgupta P, Aitken JF, Condon J, Garvey G, Whop LJ, DeBats C, Baade PD. Temporal and area-level variation in prevalence of high-grade histologically confirmed cervical abnormalities among Indigenous and non-Indigenous women, Queensland, Australia, 2008-2017. Journal of Medical Screening. 2021. doi: 10.1177/0969141320984199:969141320984199.